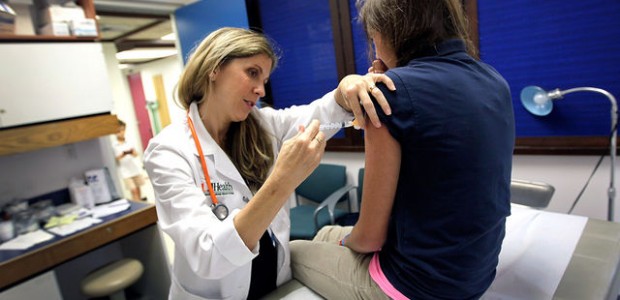
Ever since introducing the vaccine for the human papillomavirus in 2006, the incidence of the cancer-causing virus among teenage girls has been reduced by 56 percent. These numbers are coming from a new clinical study, and they are causing quite the stir in medical community.
The human papillomavirus (HPV) is a sexually transmitted disease that can lead to genital warts, cervical cancer, and even throat cancer. The CDC suggests that all girls should be given this vaccine at age 11 or 12 in order to prevent an infection which could cause cancer 2 to 4 decades later in their lives.
The Incidence of HPV in the United States
There are an estimated 79 million Americans, most of them between 15 and 25 years of age, that have contracted HPV. There are nearly 14 million new cases diagnosed each year, and about 19,000 women in the U.S. will develop cancer as a result of their infection each year (cervical cancer is the most common). While this virus also causes cancer in men, the annual rate is much lower than what’s seen in women (only about 8,000 new cases each year). In 2011, the CDC suggested that boys over the age of 11 should be vaccinated against HPV. Young adults in their early twenties or late teens can also get vaccinated if they have never received it before.
Some health care experts have expressed concern that only one-third of girls aged 13 to 17 have actually gotten the full three HPV vaccine injections. For many, this low number of full course vaccinations mean a lot of tragedies that could have been prevented. Based on the numbers, there are thousands of girls that will develop cancer at some point in their lives because health care providers were not able to hit the goal of 80 percent vaccination rates. Each year that they can’t reach these goals will mean more girls who may not be protected from cancer.
Positive Effects From the New HPV Vaccine
This study took data from the National Health and Nutrition Examination Survey to compare the number of girls and women (ages 14 to 59) who contracted HPV before the vaccine to the number contracting HPV after the vaccine was implemented. For all women and girls ages 14 to 19, the rate of infection had dropped by 56 percent from where it was during 2003-2006 to 2007-2010.
As of now, there is still questions as to how this vaccine was able to produce such a big decline, given that only 46 percent of girls have gotten a single dose and only 32 percent have completed the full course of vaccination. One theory is that this decline could be explained by what is referred to as herd immunity, where the introduction of vaccinated individuals limits the overall incidence of viral infection in a population, which in turn reduces overall infection rates. Either way, this decline is unanimously viewed as very positive.
Why Are We So Far Behind?
Currently, the U.S. lags behind other developed countries when it comes to the number of teens who are vaccinated. In Australia for example, the vaccination rate for teenage girls is as high as 80 percent. Australian health officials have reported very significant drops in the incidence of genital warts and abnormal Pap smear results, which could be an early indication for cancer.
Unfortunately in the States, there is a negative stigma surrounding the vaccination of teenage girls for a virus that is sexually transmitted. There are still many parents that believe this type of thing would actually encourage more sexual activity amongst their teens. Health care workers are trying to help these parents understand that this vaccine is meant to protect their children when they become adults.
Americans Still Uncomfortable When It Comes to the Topic of Sex
“We vaccinate well before people are exposed to an infection,” says Thomas Frieden, director of the Centers for Disease Control and Prevention. “We vaccinate for measles, for example, early in childhood or infancy because that’s well before a child may get exposed. Similarly, we want to vaccinate children well before they may get exposed.”
Unfortunately, there are a significant number of Americans that still have this general discomfort when it comes to the topic of sex, and this could be one of the primary reasons why the vaccine is not used as broadly here as in other countries. The American Cancer Society and the CDC are working together in order to help change this type of thought process.